The venous system of the legs
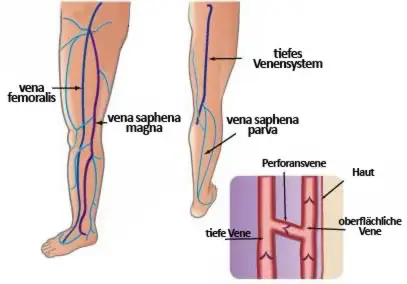
The venous system is a network of vessels consisting of superficial and deep veins and their connections (perforating veins). Every day, the veins transport about 7,000 litres of oxygen-deficient blood back to the heart – mostly against gravity.
90% of the blood is transported in the deep veins, only 10% in the superficial veins. Therefore, superficial, diseased veins can also be removed.
Varicose Veins
Varicose veins, medically called varices, are pathologically altered veins of this system.
The most important veins for the treatment of varicose legs are the following superficial truncal veins
- Vena saphena magna (large rose vein) and the
- Vena saphena parva (small rose vein)
with their respective side branches.
The visible varicose veins are the side branches of the diseased truncal veins.
Cause of varicose veins
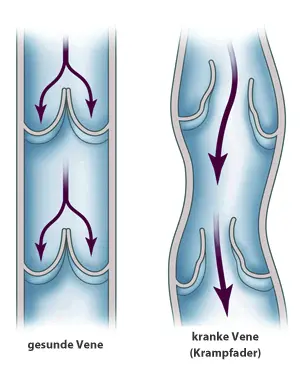
In healthy veins, opening and closing valves allow blood to be transported against gravity back to the heart. If these valves lose their ability to close, reflux occurs.
This causes the veins to dilate, become longer and become tortuous. This creates the typical picture of varicose veins (varicosis).
The development of varicose veins (varicosis) is hereditary. Approximately 20% of the western population suffer from vein changes. The spectrum ranges from spider veins to the open leg (ulcus cruris).
Additional factors such as age, gender (women are more frequently affected), pregnancies and overweight favour the development of varicose veins or can make the condition worse.
Why some people develop varicose veins and others do not is still not clear.
Clinical pictures
Over time, the chronic overpressure leads to increased leakage of fluid, protein and blood cells into the surrounding tissue. This results in inflammation, swelling (oedema), hardening (sclerosis) and brownish discolouration (hyperpigmentation) of the skin, mainly in the so-called gaiter zone above the ankle joint.
Inflammation in these diseased veins leads to superficial leg vein thrombosis (varicophlebitis), which in rare cases can result in deep leg vein thrombosis and pulmonary embolism.
In the case of prolonged courses, skin and fatty tissue are so poorly supplied with blood that this can lead to an open leg (ulcus cruris).
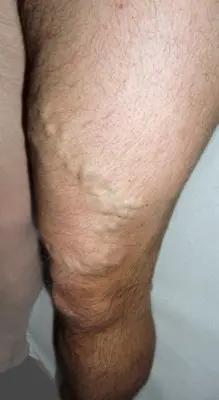
Varicose veins
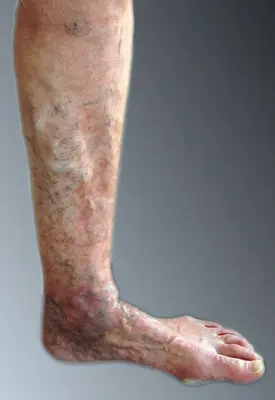
Hyper pigmentation
Recurrent varices
Recurrent varicose veins are varicose veins that reappear after months or years after successful treatment. The frequency of recurrence is about 20%. Recurrences can come directly from the groin or back of the knee, or only affect lateral branches of the upper and lower leg.
The cause is a genetic predisposition. Recurrences can also be caused by improper therapy.
Depending on the findings, these newly occurring varices can be treated by surgery (recurrent surgery in the groin), phlebectomy or foam sclerotherapy. Endovenous procedures such as laser therapy or Venefit ClosureFast can also be used.
Recommendation
All varicose vein patients should consult a vein specialist periodically. In this way, newly occurring, pathological changes in the veins can be detected in their early stages and immediately treated on an outpatient basis with a small procedure under local anaesthetic or foam sclerotherapy (hook method, foam sclerotherapy, endovenous procedures).
Diagnostics
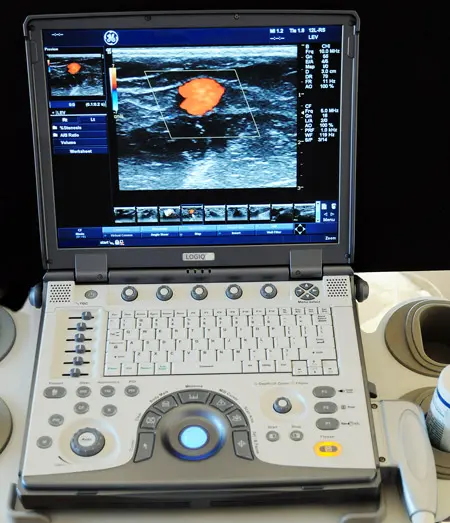
The gold standard of diagnostics in phlebology today, in addition to anamnesis and clinical examination, is colour-coded duplex sonography (ultrasound).
It allows the stages of the venous disease to be precisely determined and a treatment plan to be determined. Therapy success and course can also be checked.
Therapy plan
The diagnosis is the basis of the individual therapy plan, which can vary greatly depending on the patient. Factors that influence the therapy plan include genetic disposition, age, living conditions, general health status and the characteristics, course and size of the diseased veins.
Sometimes several procedures are used at the same time.
The aim is to completely remove all diseased veins in order to prevent recurrence.

